MSSP Quality Scoring for 2024
In the Medicare Shared Savings Program (MSSP), quality scores dictate what an ACO’s final sharing rate will be and what losses will be owed (if applicable). Beginning with the performance year (PY) 2022 and subsequent years, ACOs who meet or exceed the quality performance standard will receive the maximum shared savings rate available in their track/model. Those who meet a lower standard can receive a portion of shared savings, the amount which is determined based on their final quality score.
Quality Performance Standard
Earning Maximum Shared Savings
ACOs must meet or exceed the quality performance standard to be eligible to share in savings they may generate. For PYs 2022 and 2023 the quality performance standard was set at the 30th percentile of the full distribution of MIPS quality scores (for ACOs and other MIPS eligible clinicians reporting quality). For PY 2024 and subsequent years, the quality performance standard is set at the 40th percentile of MIPS quality scores. Starting in 2024, CMS will calculate the quality performance standard based on historic MIPS quality scores rather than using performance period data to establish the quality performance standard. NAACOS advocated for this change, which will allow ACOs to know this critical performance target in advance of the performance year starting.
Earning a Portion of Shared Savings
For ACOs who do not meet the quality performance standard to share in savings at the maximum sharing rate, there is a lower standard that if met will allow the ACO to share in a portion of savings determined based on the final quality score. If an ACO can meet or exceed the 10th percentile on an individual quality measure benchmark for at least one of the outcome measures listed in the measure set, the ACO’s final sharing rate would be scaled by multiplying the maximum sharing rate for the ACO’s track/level by the ACO’s final quality score (including any bonus points).
As a hypothetical example, an ACO participating in Basic Track Level B met the minimum savings rate and qualifies for shared savings with a final quality score of 45 points. This score is less than the 30th percentile of MIPS quality performance category scores of 67 points. Therefore, the ACO will not receive the maximum shared savings rate. The ACO did achieve a quality performance score higher than the 10th percentile for an individual measure benchmark on one of the outcome measures, therefore, the ACO is eligible to share in a portion of the savings. The shared savings rate in this example would be 40 percent (maximum sharing rate for Basic Track Level B) x 45 percent (final quality score) = final sharing rate of 18 percent.
Calculating the Quality Performance Standard
Instead of using performance period data to establish the quality performance standard, starting in PY 2024 and for subsequent years CMS will use a three-year rolling average of historical performance data with a lag of one performance year to establish the quality performance standard.
For 2024, the quality performance standard is based on MIPS quality performance category scores from PY 2020 through PY 2022 and equals 77.05 points. This CMS resource provides more information.
eCQM/MIPS CQM Reporting Incentive
CMS established the eCQM/MIPS CQM reporting incentive (a lower quality performance standard) to continue encouraging ACOs to report via all payer eCQMs and MIPS CQMs. An ACO will be deemed to have met the Quality Reporting Standard to qualify for sharing in savings at the maximum shared savings rate if the ACO:
- Reports all of the eCQMs in the APP Plus quality measure set applicable for the PY and meets data completeness for all eCQMs, and;
- Achieves a quality score equal or higher than the 10th percentile (individual measure benchmark) on at least one of the four outcome measures in the measure set, and;
- Achieves a quality score equal to or higher than the 40th percentile (individual measure benchmark) on at least one of the remaining measures in the measure set.
40th Percentile MIPS Quality Performance Category Scores Provided by CMS
| Performance Year | 40th Percentile of the MIPS Quality Performance Category Score |
| 2020 | 75.59 |
| 2021 | 77.83 |
| 2022 | 77.73 |
| 2023 | Skipped due to one year lag |
| 2024 | 77.05 |
Refer to Table 30 of the final 2024 Medicare Physician Fee Schedule rule for more detail.
Calculating an ACO’s Final Quality Score
CMS will determine an ACO’s achievement points earned for each individual quality measure in the measure set by comparing the ACO’s performance on the measure to the established benchmark for the measure. Individual measure benchmarks vary based on the reporting method being used and are established in advance of the performance year. ACOs in the first year of their contracts are provided with full credit so long as the ACO completely and accurately reports all quality measures to CMS (pay-for-reporting). Each subsequent year, the ACO will be assessed on quality measure performance for each prescribed measure in the measure set (pay-for-performance).
Example: Benchmarks by Decile for #236, Controlling High Blood Pressure
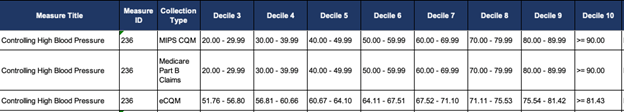
CMS then sums the total achievement points for all measures to create a total quality score. Finally, CMS adds any bonus points (if applicable) including a new quality equity bonus available beginning in PY 2023 and subsequent years, to calculate a final quality score for the ACO. This final quality score is the score that must meet or exceed the quality performance standard in order to be eligible to share in savings at the maximum shared savings rate available.
Suppressed Quality Measures Scoring Policy
In the final 2024 Medicare Physician Fee Schedule rule, CMS also made changes to its scoring policy for suppressed quality measures. This is a favorable change NAACOS advocated for and will allow more ACOs to achieve shared savings. In circumstances when the ACO’s total achievement points used to calculate the quality score for the performance year was reduced due to measure exclusion/suppression policies in MIPS, CMS will award the higher of an ACO’s own quality performance score or the 40th percentile MIPS quality performance category score when determining whether the ACO meets the quality performance standard required to share in savings.
To be eligible, an ACO must:
- Report all required measures under the APP and
- Meet data completeness requirements.
Health Equity Bonus Point Calculations
Beginning in PY 2023, CMS established a health equity adjustment that awards bonus points to the quality performance score for ACOs delivering high quality care to underserved populations. The bonus points are only available to ACOs reporting eCQMs or MIPS CQMs (and Medicare CQMs beginning in 2024). Specifically, up to 10 health equity bonus points will be added to the total quality score for qualifying ACOs with the total quality score not to exceed 100 points. The number of bonus points earned will be based on the ACO’s performance on quality measures and the population served by the ACO. The bonus points will be applied only in certain MSSP calculations, such as the quality performance standard determinations, calculations of shared savings/losses, and extreme and uncontrollable circumstances policy calculations.
To determine an ACO’s health equity adjustment bonus points, CMS will conduct the following steps:
- Calculate the performance measure scaler. The scaler is calculated for each measure, thus an ACO may fall into a different performance group for each measure. For the CAHPS measure and claims-based measures, ACOs will be compared to all ACOs performance on those measures. For all other measures performance is evaluated on ACOs reporting eCQMs/MIPS CQMs. The ACO’s measure performance scaler is the sum of the points for each of the six measures; the maximum total scaler is 24.
- Top third performing ACOs awarded scaler of 4.
- The middle third performing ACOs awarded scaler of 2.
- The bottom third performing ACOs awarded scaler of zero; ineligible to receive health equity bonus points for this measure.
- Calculate the ACO’s underserved multiplier for each ACO. CMS will use the higher value of:
- The proportion of an ACO’s assigned beneficiary population residing in a census block group with Area Deprivation Index (ADI) national percentile rank of 85 or higher,
- The proportion of an ACO’s assigned beneficiary population that are dually eligible for Medicare and Medicaid, or
- The proportion of assigned beneficiaries enrolled in the Part D Low Income Subsidy (LIS).
If an ACO has less than 20 percent of its population in any category, the ACO is ineligible for the health equity bonus points
- Calculate the ACO’s health equity bonus points. The ACO’s performance measure scaler (up to 24 points) is multiplied by the ACO’s underserved multiplier. The bonus points are capped at 10.
- For example, an ACO that is a high performer across all six measures (performance scaler of 24) with half of the population served being dual-eligible beneficiaries (underserved multiplier of 0.5) would have health equity bonus points of 12. Therefore, the bonus points would be capped at 10.
The health equity quality bonus points are available for ACOs reporting eCQMs/MIPS CQMs only. CMS will incorporate the health equity adjustment into quality performance reports for eligible MSSP ACOs. CMS will show the calculation of the health equity adjustment, including dual eligibility, LIS, and ADI data for all ACOs that report on eCQM/MIPS CQM measures even if the adjustment would not affect the determination of shared savings/losses.
In 2024, CMS revised calculations used to award health equity quality bonus points to ACOs for 2024. Under the new approach, CMS will:
- Remove beneficiaries who do not have a numeric national percentile rank available for ADI from the health equity adjustment calculation for PY 2023 and subsequent years (will not appear in the numerator or denominator) and
- Modify the calculation of the proportion of assigned beneficiaries dually eligible for Medicare and Medicaid and the calculation of the proportion of assigned beneficiaries enrolled in the LIS to use the number of beneficiaries rather than person years, starting in PY 2024.
These changes are intended to bring greater consistency between the calculation of the proportion of ACOs’ assigned beneficiaries residing in a census block group with an ADI national percentile rank of at least 85 and the proportion of the ACOs’ assigned beneficiaries who are enrolled in a Medicare Part D LIS or are dually eligible for Medicare and Medicaid.
Sharing Feedback with ACOs on Performance
CMS provides a preview of the quality score via the QPP portal. ACOs get preliminary access to results with the QPP quality submission. Final quality scores are shared via the financial reconciliation package, which is accessed through the ACO Management System (ACO-MS) data hub.
MIPS Errors and ACO Financial Determinations
MSSP shared savings and loss calculations are tied to whether an ACO meets the established quality performance standard, which is calculated based on the distribution of MIPS quality performance category scores. CMS has sole discretion to make corrections to a prior performance year’s MSSP ACO financial determinations as a result of corrections made to MIPS quality performance category scores. Typically, CMS provides MSSP financial reconciliation reports in August of the year following the performance year, with payments to ACOs initiated in September.
The timeline for conducting MIPS targeted review may extend past the date CMS issues financial reconciliation reports. Accordingly, CMS may learn of MIPS quality performance calculation errors after MSSP initial financial performance determinations are issued. CMS notes where possible, it would seek to adjust the shared savings payment or shared loss recoupment for the ACO as part of the reconciliation for a subsequent performance year. This approach would not alter the current requirement that ACOs repay shared losses within 90 days after notification of the initial determination of shared losses. NAACOS will closely monitor this process and the impact of MIPS scoring errors on ACO payment determinations and advocate for minimal disruption to ACOs.
Extreme and Uncontrollable Circumstances Policy for ACO Quality
Under the Extreme and Uncontrollable Circumstances policy, an affected ACO that fails to report quality data or reports but fails to meet data completeness or case minimum requirements will have its quality score set to the quality performance standard (i.e., achieves the maximum shared savings rate). An ACO affected by an extreme and uncontrollable circumstance that meets the alternative (lower) quality performance standard would continue to qualify for the maximum sharing rate for its track/level rather than receiving a sharing rate scaled based on the ACO’s quality performance.
